Medical students and interns face a daunting challenge: constructing accurate differential diagnoses under time pressure while managing cognitive overload. Studies show diagnostic errors contribute to 10% of patient deaths, often stemming from flawed reasoning processes. Mastering a structured differential diagnosis workflow, augmented by AI-driven clinical tools, transforms this challenge into an opportunity for enhanced accuracy and confidence. This guide walks you through a proven 2026 workflow that integrates AI as your cognitive teammate, helping you generate comprehensive differentials, prioritize critical diagnoses, and avoid common pitfalls that derail clinical reasoning.
Table of Contents
- Preparation: Gathering Essentials For A Successful Differential Diagnosis
- Execution: Stepwise Differential Diagnosis Workflow With AI Integration
- Troubleshooting And Common Pitfalls In Differential Diagnosis Workflows
- Expected Results And Practical Tips For Mastering Differential Diagnosis Using AI
- Boost Your Differential Diagnosis Skills With MedCompanion Pro
- Frequently Asked Questions
Key takeaways
| Point | Details |
|---|---|
| Structured workflows reduce errors | Following systematic steps improves diagnostic accuracy and minimizes cognitive biases that lead to missed diagnoses. |
| AI tools enhance clinical reasoning | Platforms like AMIE and iatroX generate ranked differential lists and flag critical conditions, boosting accuracy from 75% to 82-85%. |
| Top 3 plus can't-miss strategy | Focus on three most likely diagnoses plus urgent conditions requiring immediate exclusion to guide efficient testing and management. |
| Human oversight remains essential | AI complements but cannot replace clinical judgment, requiring active verification and context interpretation to prevent automation bias. |
| Iterative reassessment refines diagnosis | Updating your differential as new data emerges prevents premature closure and catches evolving presentations. |
Preparation: gathering essentials for a successful differential diagnosis
Before diving into differential diagnosis generation, you need solid groundwork. Comprehensive history and physical exam form the foundation of accurate clinical reasoning. Spend adequate time gathering chief complaint details, reviewing systems, exploring past medical history, and conducting a thorough physical examination. Document findings clearly so you can reference them throughout your diagnostic process.
Organize your clinical data systematically. Create a problem list highlighting key symptoms, physical findings, and relevant lab abnormalities. This structured approach prevents information overload and helps you spot patterns. Many students find it helpful to use a standardized template that captures presenting symptoms, timeline, associated features, and pertinent negatives.
Familiarize yourself with diagnostic frameworks before encountering complex cases. The VINDICATE mnemonic covers Vascular, Infectious, Neoplastic, Degenerative, Inflammatory, Congenital, Autoimmune, Traumatic, and Endocrine causes. This systematic approach ensures you consider broad diagnostic categories rather than fixating on obvious possibilities. Other useful mnemonics include VITAMIN CDE and the surgical SIEVE framework.
Prepare your AI tools in advance. Platforms like MedCompanion Pro integrate seamlessly into clinical workflows, offering real-time differential diagnosis suggestions and red-flag alerts. Set up your account, familiarize yourself with the interface, and understand how to input clinical data efficiently. Having these tools ready eliminates friction when you need them most.
Establish your clinical question framework. Define what you're trying to diagnose: Is this acute or chronic? Life-threatening or benign? Organ-specific or systemic? Clear framing guides your differential generation and prevents scope creep that wastes time on irrelevant possibilities.
Pro Tip: Before seeing patients, practice generating differentials for common chief complaints using VINDICATE. This builds mental templates that accelerate real-world clinical reasoning and reduce cognitive load during high-pressure situations.
Execution: stepwise differential diagnosis workflow with AI integration
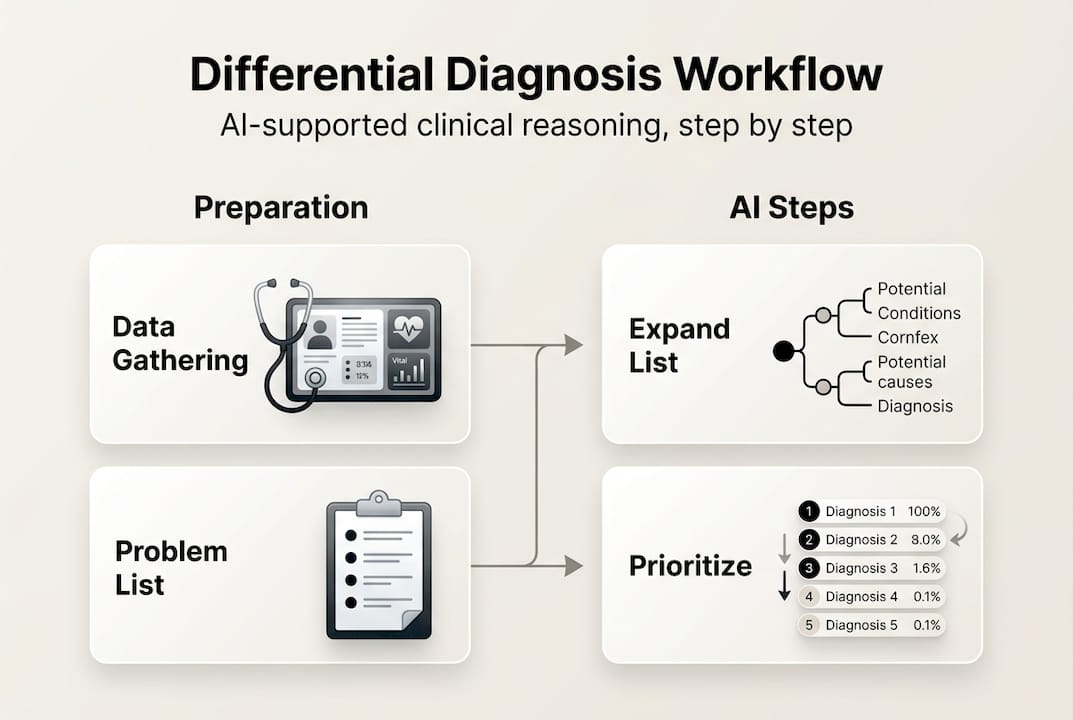
Once prepared, follow this systematic workflow to construct and refine your differential diagnosis. The process involves generating broad possibilities, prioritizing by severity and likelihood, narrowing with targeted investigations, and iterating based on new data. Each step builds on the previous one, creating a logical progression from uncertainty to diagnostic clarity.
Step 1: Generate a broad differential using systematic frameworks. Apply VINDICATE or similar mnemonics to your patient's presentation. For a 45-year-old with chest pain, consider vascular causes like acute coronary syndrome, infectious causes like pneumonia, inflammatory conditions like pericarditis, and so forth. Aim for 8 to 12 initial possibilities covering common and rare diagnoses. This breadth prevents premature narrowing that leads to missed diagnoses.
Step 2: Prioritize using the Top 3 plus can't-miss approach. Identify the three most likely diagnoses based on epidemiology, patient risk factors, and clinical presentation. Then add any life-threatening conditions you must rule out regardless of probability. For chest pain, your top three might include musculoskeletal pain, gastroesophageal reflux, and anxiety, while your can't-miss list includes myocardial infarction, pulmonary embolism, and aortic dissection.
Step 3: Engage AI tools for hypothesis expansion and validation. Input your clinical data into AI-powered platforms that generate ranked differential lists. Research shows AI-assisted workflows improve diagnostic accuracy from 75% to 82-85% by catching overlooked possibilities and highlighting red flags. Review the AI-generated list against your own reasoning, noting discrepancies that warrant investigation.

Step 4: Narrow your differential through discriminating features. Identify key questions, physical exam maneuvers, or tests that distinguish between competing diagnoses. For chest pain, an electrocardiogram and troponin level differentiate cardiac from non-cardiac causes. AI tools suggest these discriminators automatically, helping you order the right tests efficiently. Focus on high-yield investigations that maximize diagnostic information while minimizing cost and patient burden.
Step 5: Iterate and update as new information emerges. Clinical presentations evolve. A patient initially appearing stable may deteriorate, or test results may reveal unexpected findings. Reassess your differential diagnosis regularly, adjusting probabilities and adding new possibilities as warranted. This iterative approach prevents anchoring bias and catches diagnoses that develop over time.
| Workflow Step | Key Action | AI Role |
|---|---|---|
| Generate broad differential | Apply VINDICATE framework | Suggests additional rare diagnoses |
| Prioritize diagnoses | Use Top 3 plus can't-miss | Ranks by likelihood and flags urgent conditions |
| Discriminate possibilities | Order targeted tests | Recommends high-yield investigations |
| Iterate with new data | Update probabilities | Alerts to evolving patterns |
Pro Tip: Document your reasoning at each step. Writing down why you included or excluded diagnoses forces explicit thinking and creates an audit trail that improves learning and accountability.
Troubleshooting and common pitfalls in differential diagnosis workflows
Even structured workflows face challenges. Cognitive biases like anchoring, availability, and premature closure derail diagnostic accuracy by causing you to fixate on initial impressions or recent cases. Anchoring occurs when you lock onto your first hypothesis and ignore contradictory evidence. Availability bias makes you overweight diagnoses you've seen recently. Premature closure happens when you stop considering alternatives after finding a plausible explanation.
Atypical presentations pose another major challenge. Classic textbook symptoms appear in only a minority of cases. Elderly patients with myocardial infarction may present with confusion rather than chest pain. Diabetic patients with infections may lack fever. Young, healthy individuals can develop serious conditions typically seen in older populations. Stay vigilant for zebras when hoofbeats don't fit the expected horse pattern.
AI tools help mitigate these pitfalls by providing breadth and flagging overlooked possibilities. However, AI complements rather than replaces human judgment, requiring active oversight to interpret suggestions contextually and catch AI errors. Algorithms trained on biased datasets may perpetuate disparities or miss conditions poorly represented in training data. Always verify AI recommendations against clinical guidelines and your own assessment.
Common troubleshooting strategies include:
- Use forcing functions like systematic review of organ systems to counter anchoring
- Consult colleagues or AI platforms for second opinions on complex cases
- Explicitly document why you're excluding diagnoses to avoid premature closure
- Maintain a personal log of missed diagnoses to identify your recurring blind spots
- Set calendar reminders to reassess stable patients rather than assuming initial diagnosis was correct
Cognitive debiasing techniques strengthen clinical reasoning. The mnemonic SLOW DOWN reminds you to Stop and think, Listen to concerns, Organize differential systematically, Watch for bias, Decide on tests, Observe response, Work with team, and Note lessons learned. This metacognitive approach transforms reactive thinking into deliberate analysis.
"The greatest enemy of diagnostic accuracy is not ignorance but the illusion of knowledge. Structured workflows and AI tools combat this by forcing us to consider what we don't know."
Pro Tip: After each clinical encounter, spend two minutes asking yourself what alternative diagnoses you might have missed and what additional questions could have improved your reasoning. This reflection builds diagnostic expertise faster than passive experience alone.
Expected results and practical tips for mastering differential diagnosis using AI
Implementing this workflow yields measurable improvements in diagnostic performance. AI-assisted approaches achieve 82-85% accuracy compared to 75% for conventional methods, translating to fewer missed diagnoses and better patient outcomes. You'll notice increased confidence in your clinical reasoning as systematic approaches replace ad hoc thinking. Documentation becomes more comprehensive and defensible, protecting you legally while improving care continuity.
The clinician-in-the-loop model balances AI strengths with human judgment. AI excels at breadth, processing vast medical knowledge instantly and flagging rare possibilities humans forget. Humans excel at context, interpreting subtle cues, incorporating patient values, and making nuanced judgments AI cannot replicate. This partnership leverages both strengths while mitigating weaknesses.
Regular practice accelerates skill acquisition. Use the Top 3 plus can't-miss framework with AI expanders on every patient encounter, even straightforward cases. This repetition builds mental models that become automatic over time. Review your differential diagnoses with attendings, comparing your reasoning to expert approaches and identifying gaps.
Leverage AI-powered quizzes and case simulations to practice without patient risk. Platforms like MedCompanion Pro offer scenario-based learning where you can test your diagnostic workflow against validated guidelines. These exercises reveal cognitive biases and knowledge gaps in a safe environment, accelerating improvement.
Guard against overreliance and automation bias. Just because AI suggests a diagnosis doesn't make it correct. Verify recommendations against clinical findings, lab results, and established guidelines. Maintain healthy skepticism, especially when AI suggestions conflict with your clinical gestalt. Your judgment remains the final arbiter.
| Approach | Accuracy | Key Advantage | Main Limitation |
|---|---|---|---|
| Conventional clinical reasoning | 75% | Contextual nuance | Cognitive biases, limited breadth |
| AI-only diagnosis | Variable | Comprehensive coverage | Lacks clinical context, prone to errors |
| Clinician-in-the-loop AI | 82-85% | Combines breadth with judgment | Requires active engagement |
Practical tips for maximizing workflow effectiveness:
- Start each shift by reviewing common presentations and their differentials to prime your memory
- Keep a differential diagnosis checklist on your phone for quick reference during clinical encounters
- Schedule weekly case reviews where you present challenging diagnoses and discuss alternative possibilities
- Track your diagnostic accuracy over time to identify improvement areas and celebrate progress
- Join online communities where medical students share diagnostic challenges and reasoning strategies
Pro Tip: Create a personal differential diagnosis library by documenting interesting cases with your initial differential, final diagnosis, and lessons learned. This becomes an invaluable study resource and helps you recognize patterns faster in future encounters.
Boost your differential diagnosis skills with MedCompanion Pro
Mastering differential diagnosis requires more than knowledge. It demands structured practice with intelligent feedback. MedCompanion Pro provides AI-powered support specifically designed for medical students and interns navigating clinical rotations. The platform generates ranked differential diagnoses based on your patient data, flags critical conditions requiring immediate attention, and suggests discriminating questions to narrow possibilities efficiently.
Unlike generic AI tools, MedCompanion Pro integrates seamlessly into your clinical workflow. Document patient encounters using guided anamnesis templates, receive real-time differential diagnosis suggestions, and generate comprehensive reports in multiple languages including English, French, Romanian, and German. The platform's case simulation library lets you practice the Top 3 plus can't-miss approach on hundreds of scenarios, building diagnostic confidence before high-stakes patient encounters. With GDPR-compliant security and end-to-end encryption, your learning remains private and protected. Start refining your clinical reasoning today with tools built specifically for your training needs.
Frequently asked questions
How do I effectively use AI tools in differential diagnosis without becoming over-reliant?
Treat AI as a cognitive forcing function rather than a decision-maker. Generate your own differential first, then compare it with AI suggestions to identify blind spots. Human oversight prevents automation bias and catches AI errors that arise from training data limitations. Always verify AI-recommended diagnoses against clinical guidelines, patient context, and your physical exam findings. Use AI platforms to expand your thinking, not replace it.
What are practical mnemonics to generate a broad differential diagnosis list?
VINDICATE covers major diagnostic categories: Vascular, Infectious, Neoplastic, Degenerative, Inflammatory, Congenital, Autoimmune, Traumatic, and Endocrine. Apply each category systematically to your patient's presentation to ensure comprehensive coverage. Alternative mnemonics include VITAMIN CDE, which adds Metabolic and Drugs/toxins, and the surgical SIEVE framework focusing on structural abnormalities. Choose one mnemonic and use it consistently until it becomes automatic.
How can I prioritize diagnoses when faced with many possible options?
Implement the Top 3 plus can't-miss strategy. Identify the three most likely diagnoses based on epidemiology, patient risk factors, and symptom patterns. Then add any life-threatening conditions requiring urgent exclusion regardless of probability. This focused approach guides efficient testing and management while ensuring safety. Consider both severity and likelihood when prioritizing, ordering investigations that maximize diagnostic yield while minimizing harm and cost.
Why is iterative reassessment important in differential diagnosis workflows?
Clinical presentations evolve as diseases progress and new data emerges. Test results, treatment responses, and developing symptoms change diagnostic probabilities significantly. Regular reassessment prevents premature closure by forcing you to reconsider your initial hypothesis against accumulating evidence. Set specific reassessment intervals based on patient acuity, updating your differential whenever new information becomes available. This dynamic approach catches diagnoses that unfold over hours or days rather than presenting fully formed at initial encounter.
